We start todays blog with a huge congratulations to Dr Luke Hughes Blood who passed his PhD viva at the end of January, completing 3 years of research in the area of blood flow restriction training. He has now started working on a 2-year funded post-doctoral position with our research group continuing his research in the area. So, before he starts with updating his current work, we asked him to give us an overview of his PhD area and the applications it may have for practitioners using blood flow restriction in rehabilitation and performance.
Left:  Dr Luke Hughes (middle) following his PhD examination, alongside his examiner’s Dr Lee Herrington & Dr Charlie Pedlar.
Dr Luke Hughes (middle) following his PhD examination, alongside his examiner’s Dr Lee Herrington & Dr Charlie Pedlar.
My cross-discipline PhD in physiology and clinical rehabilitation focused on the use of blood flow restriction (BFR) resistance training as a clinical rehabilitation tool. BFR resistance training involves partial restriction of arterial blood inflow and full restriction of venous blood outflow in the exercising limb. This is achieved by placing a type of blood pressure cuff around the proximal limb and inflating it to a set pressure to cause compression of the underlying vasculature, which creates an ischemic and hypoxic environment in the muscle tissue. BFR resistance training can stimulate muscle hypertrophy and strength adaptations using a light external load of ~30% of one repetition maximum (1RM). This makes it an attractive rehabilitation tool for load-compromised populations. The overall aim of my thesis was to examine the use of BFR resistance training as a clinical training tool for rehabilitation of patients following anterior cruciate ligament reconstruction (ACLR) surgery in the progressive limb loading phase of rehabilitation.
I started by conducting a systematic review and meta-analysis of the existing literature to 1) determine the effectiveness of BFR training on muscle strength in different load compromised populations, and 2) identify important aspects related to application of this technique. This review determined that BFR is an effective alternative to heavy load (HL) resistance training for improving muscle strength. It also highlighted important issues regarding BFR application that may influence the safety and effectiveness of the BFR stimulus. It was published in the British Journal of Sports Medicine (Hughes et al. 2017) and was followed by publication of an editorial paper in the same journal (Patterson et al. 2017). Following these papers, I wrote a review paper discussing how BFR resistance training may be implemented within ACLR rehabilitation specifically, which was published in Techniques in Orthopaedicsas part of a symposium on BFR (Hughes et al. 2018).
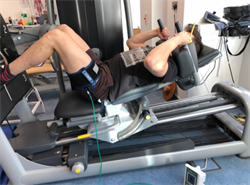
An example of BFR during leg press resistance exercise.
In the initial two experimental studies, I set out to address issues identified from the systematic review related to the safety and effectiveness of the BFR stimulus. Study one was designed to determine the most appropriate device for BFR application, by examining the cuff to limb interface pressure, perceptual and hemodynamic response to an acute bout of BFR resistance exercise. The results of this study demonstrated that a device that could effectively control and regulate pressure during BFR resistance exercise minimised the perceptual and hemodynamic responses to exercise. This paper was published in the Scandinavian Journal of Medicine and Science in Sport(Hughes et al. 2018). Study two investigated the influence of different body positions on limb occlusion pressure measurement (LOP), which provides a method of individualising the prescription of BFR pressure. This study found that LOP is dependent on body position, and was published in the journal PeerJ (Hughes et al. 2018). The results of these initial two studies informed the subsequent clinical studies on the basis that, to ensure a safe and effective BFR stimulus, LOP must be measured in the body position that exercise will be performed and BFR must be applied using a device that can effectively control pressure.
Alongside completion of these initial two studies I had applied for NHS ethical approval to conduct clinical experimental studies in ACLR patients within the NHS. Before conducting a training study, I set out to determine if BFR resistance training would be feasible to use as a training tool in ACLR patients in the manner I had planned. This involved examination of the acute physiological responses during a post-surgery setting. The results of this NHS study indicated that, in ACLR patients following surgery, the perceptual and hemodynamic responses to BFR resistance exercise were no greater than HL resistance exercise, and BFR resistance exercise reduced pain both during and for 24 hours post-exercise. From these findings it was determined that BFR resistance training would likely be feasible during a post-surgery training programme in these patients, and this study was published in Physical Therapy in Sport (Hughes et al. 2018).
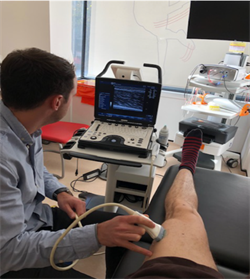 Muscle morphology measurements using ultrasonography.
Muscle morphology measurements using ultrasonography.
The final PhD data collection was an 18 month clinical randomised controlled trial in the NHS, which examined the effectiveness of BFR resistance training during the post-surgery rehabilitation of ACLR patients compared to HL resistance training, which was the standard care in the NHS setting in which the study was conducted. I investigated the effect on muscle hypertrophy, strength, physical function, knee pain and effusion over an eight week post-surgery rehabilitation programme (study four), alongside examination of the safety and feasibility (study 5). Using a criteria-driven approach, patients underwent an 8 week resistance training programme consisting of either BFR resistance training or HL resistance training alongside standard rehabilitation in the progressive limb loading phase of rehabilitation. The results of study four showed that BFR resistance training can improve skeletal muscle hypertrophy and strength to a similar extent as HL resistance training with a greater reduction in knee joint pain and effusion, leading to greater overall improvements in physical function. From study five it was evident that pain was lower during training and on the subsequent day with BFR resistance training. Moreover, the perceptual responses to BFR resistance training were similar to HL resistance training, thus do not limit application in a post-surgery rehabilitation setting. Importantly, no adverse effects in generaloron knee joint laxity were observed.
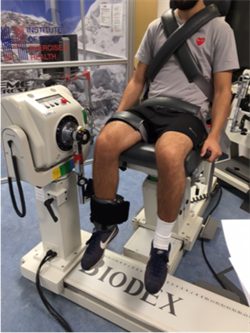 Assessment of isokinetic strength.
Assessment of isokinetic strength.
Overall, this thesis demonstrated for the first time that BFR resistance training can stimulate comparable skeletal muscle hypertrophy and strength adaptations and greater improvements in physical function, pain and effusion compared to standard care HL resistance training in ACLR patients during the progressive limb loading phase of rehabilitation within the NHS. Moreover, this thesis demonstrated that BFR resistance training is a feasible training tool and can reduce knee pain to a greater extent via the use of light external loads and/or a pain-modulating effect. This thesis gave rise to some key points to consider in the application of BFR in clinical rehabilitation, including:
- LOP measurement must be performed in the body position that BFR exercise will be performed to ensure accurate BFR pressure prescription.
- The perceptual and hemodynamic responses to BFR exercise are minimised when using a BFR device that effectively controls and regulates pressure.
- The perceptual and hemodynamic responses to BFR resistance exercise in ACLR patients do not limit application in a post-surgery setting.
- BFR resistance training reduces knee joint pain during and after exercise, resulting in a greater overall reduction in pain throughout a rehabilitation programme.
- BFR resistance trainingis feasible and can improve skeletal muscle hypertrophy and strength to a similar extent as HL resistance trainingduring the progressive limb loading phases of ACLR rehabilitation.
- BFRresistance traininghas a pain-modulating effect but requires further investigation to determine the mechanisms and establish the time course of this response.